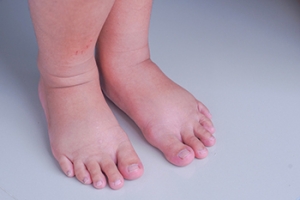
Lymphoedema and Swelling of the Feet
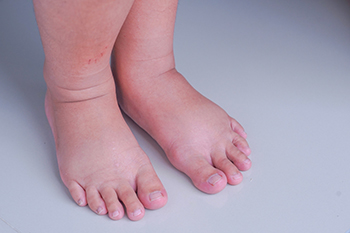
Lymphoedema is a condition where the legs or feet swell due to fluid buildup because the body's lymphatic system, which functions similarly to veins, is struggling to remove it. This swelling is called edema and can happen when you do not move enough, such as after sitting for long periods during a flight. Persistent swelling of the feet, swelling that lasts over three months, is known as chronic edema, which suggests the beginning of lymphatic failure or early lymphoedema. If left untreated, chronic foot edema can cause skin changes, deeper tissue damage, and increase the risk of infections such as cellulitis. It is often associated with chronic venous insufficiency. Various factors can contribute to lymphoedema, including genetics, obesity, inactivity, vein problems, or damage from cancer treatments. Joint surgery may also impair lymphatic vessels, leading to lymphoedema. If you are experiencing swollen feet on a regular basis, it is suggested that you make an appointment with a podiatrist as quickly as possible to obtain treatment and prevent serious complications.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact Jennifer M. Kern, DPM of South Carolina. Our doctor can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
- Phlebitis - A condition that causes the veins to become inflamed and can also cause leg pain.
- Liver disease - This may lead to low blood levels of albumin which is a protein. This can cause fluid in the blood to pass into the tissues and several areas of the body can become swollen.
- Heart failure - When the heart doesn’t pump properly the blood that is normally pumped back to the heart can pool in the veins of the legs causing swollen feet.
- Kidney disease - One of the main functions of the kidneys is releasing excess fluid in the body. This type of condition can make it difficult for the kidneys to function properly, and as a result the feet may become swollen.
- Deep-vein thrombosis (DVT)- This is a serious condition where blood clots form in the veins of the legs. They can block the return of blood from the legs to the heart which may cause the feet to swell. It is important to be treated by a podiatrist if this condition is present.
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated.
If you have any questions please feel free to contact our office located in West Columbia, SC . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Swelling of the Feet
There are many reasons why patients experience swelling of the feet. It is rather common and may be a side effect of pregnancy or from sitting and standing for most of the day. Gravity could also play a role in the development of swollen feet. It is known that the weight of blood volume in our bodies is exerted on the veins in the legs and feet. The veins may not work as efficiently during the aging process, and this could make the blood flow backward causing swollen feet. Relief may be found when obese patients lose weight, and it may help to engage in compression therapy by wearing compression socks, stockings, or athletic sleeves. This method can release pressure on the feet and ankles which may help to reduce existing swelling. There are patients who have controlled their swollen feet by implementing healthy lifestyle changes. These can consist of reducing salt intake, incorporating a gentle exercise regime into the daily routine, and drinking plenty of fresh water. Swollen feet may be a temporary condition that affects people who travel via airplane or automobile, so it is beneficial to walk as frequently as possible even though it can be difficult. Swelling of the feet can also be indicative of other health issues so it is important to pay attention to any type of chest pain, mental confusion, dizziness, or fever. If you consistently have swollen feet, it is strongly suggested that you consult with a podiatrist who can help determine the cause and how to effectively treat it.
Conditions That May Require Foot Surgery
Managing persistent foot pain or deformities can be challenging, often prompting the consideration of foot surgery when conservative treatments prove ineffective. In such cases, surgery becomes a viable option. Bunions, or hallux valgus, can be surgically managed when conservative treatments fail to alleviate pain and hinder day-to-day functioning. Similarly, hammertoes may necessitate surgery when they become rigid and painful, causing issues such as inflammation and open wounds. Metatarsal surgery addresses various foot issues caused by conditions like rheumatoid arthritis, fractures, and dislocated joints. Ankle osteoarthritis, marked by symptoms such as pain, stiffness, and swelling, may require surgical intervention. Achilles tendon disorders, including tendonitis, may prompt surgery consideration. Morton's neuroma, characterized by nerve thickening between the third and fourth toes, might necessitate surgery for those unresponsive to non-surgical management. Posterior tibial tendon dysfunction, or adult-acquired flatfoot, may require surgical intervention as symptoms worsen, aiming to restore the function of the posterior tibial tendon and support the arch. Foot surgery is generally considered a last resort, but it can be a consideration when conservative treatments no longer provide relief for persistent foot pain or deformities. It is suggested that if you are suffering from continual foot, toe, or ankle pain that you schedule an appointment with a podiatrist to determine whether surgery is the appropriate course of action for you.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact Jennifer M. Kern, DPM of South Carolina. Our doctor will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact our office located in West Columbia, SC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot Surgery
In most cases, foot surgery is often chosen as the last available option for conditions that have otherwise been unsuccessfully treated. Surgery may be necessary for several reasons, including the removal of foot deformities (e.g. bone spurs or bunions), arthritis problems, reconstruction due to injury, and congenital malformations (e.g. club foot or flat feet). Regardless of one’s age, foot surgery may be the only successful option for treatment for certain conditions.
The type of surgery one undergoes depends on the type of foot condition the patient has. For the removal of a bunion growth, a bunionectomy is necessary. If the bones in the feet need to be realigned or fused together, a surgical fusion of the foot is needed. For pain or nerve issues, a patient may require surgery in which the tissues surrounding the painful nerve are removed. Initially, less invasive treatments are generally attempted; surgery is often the last measure taken if other treatments are unsuccessful.
While in many cases surgery is often deemed as the final resort, choosing surgery comes with certain benefits. The associated pain experienced in relation to the particular condition is often relieved with surgery, allowing patients to quickly resume daily activities. The greatest benefit, however, is that surgery generally eliminates the problem immediately.
Podiatry history has shown that foot treatments continue to evolve over time. In the field of foot surgery, endoscopic surgery is just one of the many advanced forms of surgery. As technology vastly improves so too will the various techniques in foot surgery, which already require smaller and smaller incisions with the use of better and more efficient tools. Thanks to such innovations, surgery is no longer as invasive as it was in the past, allowing for faster and easier recoveries.
What Is Involved in a Diabetic Foot Exam?
A diabetic foot exam is a comprehensive evaluation essential for managing diabetes and preventing foot-related complications. During this examination, podiatrists visually inspect the feet for any cuts, sores, blisters, or signs of infection. They also check for changes in skin color, swelling, and redness. Another critical aspect of the exam involves assessing sensation in the feet. Podiatrists use tools like a monofilament or tuning fork to test for diabetic neuropathy, a condition that can reduce sensitivity in the feet. To evaluate blood flow, pulses in the feet are checked to identify any circulation problems that may slow down wound healing. Additionally, podiatrists look for foot deformities, such as bunions or hammertoes, which can increase the risk of pressure sores. An examination of the patient’s shoes will be done to ensure proper fit and support. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist for such exams, as well as to get vital education on how to take care of your feet to preserve their health.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Jennifer M. Kern, DPM from South Carolina. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in West Columbia, SC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Care for Diabetic Foot
Millions of people are affected by diabetes each year. Diabetes damages blood vessels in all parts of the body, especially the feet. The legs and feet may develop slow blood flow, which causes neuropathy, or nerve damage. Once a diabetic patient develops neuropathy, it is important that the feet are well taken care of. Otherwise, the lower limbs may have to be amputated. This only happens in drastic cases, but it shows how seriously diabetic foot care should be taken.
It is very important to always wash and dry the feet thoroughly, especially in between the toes, if you’re a diabetic. Secondly, examining your feet and toes for redness or sores must be done, even if you do not feel pain. You may also want to examine your feet from the bottom. Try to avoid wearing colored socks to prevent infections that may occur from the dye. Well-fitting socks are also highly recommended.
A diabetic’s physician should always monitor their blood levels to test how well blood sugars are being maintained. In addition to giving advice about everyday eating habits and foot care, a physician may prescribe medicine to help with the diabetic patient’s neuropathy. It is also advised to see a podiatrist if experiencing any feet conditions. Toenails may also need to be taken care of by a podiatrist. This prevents patients from cutting too deeply around their cuticles, which can lead to infection.
A person can take care of their feet at home by following the instructions of their physician. Using creams on one’s feet is also an effective way to heal dryness. Proceed with caution when using tools to remove calluses, as severe diabetics may not be able to feel pain on their feet. If any complications arise do not hesitate to contact a podiatrist.
On a daily basis, diabetic feet must be checked. If you are ever concerned about something, contact your health care professional. You never want to wait until a wound becomes too severe to treat. If left untreated, gangrene may develop. Gangrene is a serious infection that can lead to sepsis or amputation. It is also important for diabetics to be on the lookout for ulcers. Ulcers are sores that develop from tissue loss on the skin. They can be quite painful and require intensive treatment. Early treatment and everyday inspection are imperative to staying healthy.
Treatment Options for a Torn Achilles Tendon
An Achilles tendon tear can be a debilitating injury, but with proper treatment, recovery is possible. The approach to treatment varies depending on the severity of the Achilles tendon tear. For partial tears, a common non-surgical option is immobilization by using a walking boot, leg brace, or splint for approximately six weeks. This restricts movement, allowing the tendon to heal correctly and prevent further damage. Using crutches may be necessary during this period to avoid putting weight on the injured ankle. Rest is an essential component of healing, along with keeping the injured leg elevated. In cases of an Achilles tendon rupture, or complete tear, surgery is likely to be necessary. Before the procedure, patients may wear a walking cast or boot to protect the injured area. During surgery, a podiatrist makes incisions down the back of the heel, reconnects the torn tendon, and stitches the wound closed. In post-surgery, patients wear a cast or splint to immobilize the tendon, with prescribed pain medication, and elevation to aid healing. If you have an Achilles tendon tear or rupture, it is suggested that you schedule an emergency appointment with a podiatrist for guidance on the proper treatment.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Jennifer M. Kern, DPM of South Carolina. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in West Columbia, SC . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
What are Achilles Tendon Injuries
The Achilles tendon is the strongest tendon in the human body. Its purpose is to connect the lower leg muscles and calf to the heel of the foot. This tendon is responsible for facilitating all types of movement, like walking and running. This tendon provides an enormous amount of mobility for the body. Any injuries inflicted to this tissue should be immediately brought up with a physician to prevent further damage.
The most common injuries that can trouble the Achilles tendon are tendon ruptures and Achilles tendinitis. Achilles tendinitis is the milder of the two injuries. It can be recognized by the following symptoms: inflammation, dull-to-severe pain, increased blood flow to the tendon, thickening of the tendon, and slower movement time. Tendinitis can be treated via several methods and is often diagnosed by an MRI.
An Achilles tendon rupture is trickier to heal, and is by far the most painful injury. It is caused by the tendon ripping or completely snapping. The results are immediate and absolutely devastating, and will render the patient immobile. If a rupture or tear occurs, operative and non-operative methods are available. Once the treatment begins, depending on the severity of the injury, recovery time for these types of issues can take up to a year.
Simple preventative measures can be taken as a means to avoid both injuries. Prior to any movement, taking a few minutes to stretch out the tendon is a great way to stimulate the tissue. Calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses are all suggested ways to help strengthen the lower legs and promote Achilles tendon health.
Many problems arise among athletes and people who overexert themselves while exercising. Problems can also happen among those who do not warm up properly before beginning an activity. Proper, comfortable shoes that fit correctly can also decrease tendon injuries. Some professionals also suggest that when exercising, you should make sure that the floor you are on is cushioned or has a mat. This will relieve pressure on the heels. A healthy diet will also increase tendon health.
It is very important to seek out a podiatrist if you believe you have an injury in the Achilles region. Further damage could result in severe complications that would make being mobile difficult, if not impossible.
Chronic Plantar Fasciitis

Plantar fasciitis is a common reason for long-lasting heel pain. It can affect both active, young people and older people who do not move as much. This condition happens when the plantar fascia, a band of tissue in the foot, is repeatedly strained. It is often linked to tight calf muscles. Podiatrists can generally diagnose this condition by talking to the patient and examining their foot. They only use imaging tests if the case is unusual or does not get better with initial treatment. The main symptom is a sore heel, especially when taking the first steps in the morning or after sitting for a while. Treatment involves changing activities and stretching the calf and foot. Special shoe inserts that support and cushion the heel can also help. If pain continues after six months, podiatrists may suggest less invasive treatments or even surgery. These treatments help the body heal itself or relieve pain. However, some injections, while they reduce pain, could also weaken the foot tissue. Surgery options involve releasing tension in the calf or making small cuts in the plantar fascia to encourage healing. If you have chronic plantar fasciitis, it is suggested that you make an appointment with a podiatrist who can determine what the best treatment options are for you.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Jennifer M. Kern, DPM from South Carolina. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in West Columbia, SC . We offer the newest diagnostic and treatment technologies for all your foot care needs.